- Home
- SLIPPED DISC
- Lumbago with leg pain
Lumbago with leg pain
Lumbago with leg pain is what most folk associate a chiropractor with; numbness and weakness in the limb are not uncommon.
This page was last updated by Dr Barrie Lewis on 15th June, 2023.
A 38 year old man consulted me six weeks ago with LBP and serious limb signs and symptoms. He was suffering primarily from severe left cramping pain in his posterior thigh and calf. The ratio was 40 to 60; in other words, less lumbago than sciatica. That's an ominous prognosis.
It all began four weeks earlier whilst kicking a rugby ball around with his children. He complained that his thigh and ankle felt weak and wobbly. There was some improvement with his doctor's anti inflammatory medication; the radiation had also been to his foot.
His condition was aggravated by turning in bed, and sneezing which elicited stabs in the limb; standing up after sitting, and walking.
Interestingly, sitting brought relief, but afterwards it was much worse.
In these severe cases, standing is often impossible, and sitting is strictly prohibited; although not desirable, intermittent bed rest with exercise is the only alternative.
Lumbago with leg pain
Lumbago with leg pain is according the research is best treated with spinal manipulation and rehabilitation with various exercises; its the biggest drain on insurance companies after cardiovascular disease and malignancies, and keeps chiropractors and surgeons in business. Think more about preventon.
Examination
Mr K is an obese man with a large belly. He reeked of tobacco.
Forward flexion provoked pain in the back of the left calf muscle. Extension of the back increased the stabs in his low back, particularly at lumbar vertebra 5.
Sacroiliac tests were negative.
The slump test for sciatica, left, level 3, provoked severe left calf pain but minimal back discomfort; he was on strong painkillers.
Slump test on the right provoked no back or leg pain.
Neurological testing: The achilles reflex on the left was totally absent.
There were no sensory changes.
There was marked weakness in three separate myotomes:
Heel and toe raising were both weak. The quadriceps was giving at the knee, all on the left.
Chiropractic examination at this lower back and leg pain casefile.
He walked with a marked limp associated with the weakness in his left leg. There were no fixations in the sacro iliac joints, but L2 and L5 were jammed up on motion palpation.
The L5 joint was tender on deep palpation.
There were no obvious piriformis or hip pathologies.
Muscle tone was generally poor. The lumbar lordosis was increased.
MRI (10 June)- taken after the 4th manipulation.
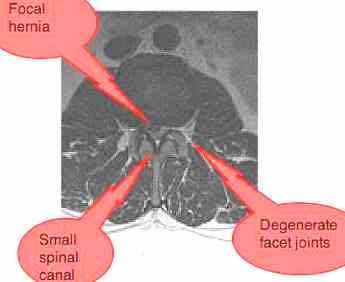
Radiological report
L1-L2: annular tear with a bulge of the disc, with narrowing of the intervertebral foramen. No nerve root compromise.
L2-L3: Focal herniation of the disc with compromise of the nerve root on the right.
L3-L4: Lumbar Stensosis: annular tear + hypertrophic facet changes + thickening of the ligamentum flavum.
L4-L5 Lumbar Stenosis, no compromise of the nerve root.
L5-S1: Moderate facet hypertrophy. No other abnormalities.
Lumbar stenosis
CONSULT 1: History, examination and first treatment
Mr K could barely rise from the chair in the waiting room, known as Minor's sign, and walked with difficulty to the examination room.
The history was routine with the exception of the fact that he had more pain in the left leg than the back, and that his leg collapsed regularly under his weight. He was unsure whether this was due to pain or frank weakness.
The examination was unusual in only one respect; there was weakness in three distinct myotomes. The gastrocnemius, extensor hallucis longus and quadriceps femoris are supplied by three different nerve roots.
The reproduction of leg pain, with no back pain, is not that unusual in the Slump test for sciatica; it just served to confirm a serious nerve impingement syndrome.
Contrary to our usual policy, because he was in so much pain, he immediately received the first treatment at the first consultation.
Consult 2; report of findings and second treatment
Diagnosis; there is a severe disc prolapse, possibly at more than one level. However, he had no symptoms in the right leg, as expected from the MRI.
Lumbar stenosis, unlikely at his age, but with a typical trefoil shaped canal is certainly a possibility. The scan is an essential tool in the management of severe nerve impingement cases. I recommend a second opinion from a neurologist.
Treatment; 2 consultations per week for 3 to 5, followed by a
vigorous programme, and an occasional, regular treatment until the
condition has stabilised, probably for two months.
Chiropractic philosophy; an explanation of the basic tenets of our treatment and the essence of his condition.
Three important issues face us.
- Taking a week or two, possibly longer, of intermittent bed rest, exercises and gentle walk every hour.
- Greatly reduced smoking, and preferably stopping completely, for the next six weeks at least. Decreased oxygenation of the damaged disc would inhibit healing.
- Weight loss and exercise are vital for a good outcome in both the short and long term.
An explanation of the high probability of initial improvement and subsequent set back within a few months, if he never went through the rehab programme.
- Lower back and leg pain exercises
Subjective: Slight but definite reduction in leg pain.
Objective: Slump test for sciatica was less positive.
Assessment: Progress. Referral letter to medical doctor for an MRI.
Treatment: sideposture manipulation of L5, lying on right side.
CONSULT 3: 3rd treatment
S: Feeling better.
O: Less pain with flexion. Slump still postive in the left leg.
A: Progress.
P: Consult with a neurologist tomorrow.
CONSULT 4
S: 10% less leg pain.
O: Slump 3 is now negative.
A: MRI reports a hernia on the RIGHT at L2-3. And lumbar stenosis in the mid and lower lumbar spine. Copy of the MRI requested.
P: Continued adjustment of L5-S1 joint, lumbar roll technique.
Neurologist is guardedly positive about chiropractic. Diagnosis given: Lumbar stenosis.
CONSULT 5
S: 50-80% less pain. Left leg feeling stronger, less "giving".
O: Range of motion of the spine improving, less pain.
A: Progress better than expected. Patient in new job, unable to take leave, and recommended bed rest. Has lost 3kg, and trying to smoke less.
P: Add adjustment of L2, lumbar roll, lying Left-side-down. First of rehab exercises.
CONSULT 6
S: Improving.
O: Ranges of motion good, guarded.
A: Excellent.
P: As before.
Leg pain sciatica
Leg pain sciatica is always a challenge for the patient and doctor alike.
CONSULT 7
S: Lower back and leg pain sciatica still improving.
O: Slump 7 completely negative. Forward bending is guarded but painfree. Patient not limping.
A: Definite improvement in the strength of the muscles in the left leg. Able to lift big toe off the ground.
P: First exercise for stability of the pelvis.
CONSULT 8
S: Slight setback yesterday, no obvious cause. Back to 50% less pain.
O: Flexion mildly painful again. Slump 7 still negative.
A: Not unexpected slight relapse with all the sitting.
P: As before. Chiropractic adjustments. Holiday 2weeks.
CONSULT 9
Mr K has almost no pain. He found swimming very beneficial, the leg is no longer collapsing at all, feeling much stronger.
Gentle bilateral mobilisation. No true manipulation. More rehab exercises.
CONSULT 10
In three weeks time. Advised wife to join him in a consult over the future. The importance of regular walking, healthy diet... behind every great man sits a great woman pulling the strings, and making sure things go according to plan.
CONSULT 11
He is doing unbelievably well. A very positive man, he has taken the radical decision to give up smoking and lose weight simultaneously; so far so good.
Lumbar stenosis
In the management of spinal
conditions like this lumbago with leg pain case, it never ceases to amaze me how
some people with very severe signs respond far quicker than expected,
whilst others with minor problems continue with nagging discomfort.
Mr K had everything going against him. Seriously overweight with poor muscle tone, a smoker, and paresis corresponding to three different nerve roots, the prognosis was very poor. Unable to take time off from a sitting job, I gave chiropractic little chance; and yet within weeks he was much improved.
He is taking the poor long term prognosis seriously, and doing his best to improve his health. He's exercising, trying to smoke less, and losing weight. A month ago he was on the verge of major invasive surgery for spinal stenosis, with all the attendant freely acknowledged attendant complications. Leg pain sciatica is an extremely painful and debilitating condition.
Clinically his case is mysterious. The hernia at L2 to 3 on the right appears to be an incidental finding. All his symptoms are on the left.
The spinal stenosis at numerous levels explains the weakness in the quadriceps muscle and the great toe dorsi flexor, but most of his symptoms, and the clinical findings relate to the L5 to S1 joint where the MRI findings are least. However, the scan was taken after 4 manipulations which may have changed the findings.
Complications of surgery
How reliable are Xrays and scans? I've learnt the hard way over the years. Decide to the best of one's ability from the physical exam where the problem is, and then look to the X-ray and MRI for confirmation. Not vice versa.
Based on the
scan I would have decided the primarily problem was at L2-L3 and would
certainly not have had the success we had. Every case of lumbago with leg pain is unique and a challenge.
The proof of the pudding is in the eating. He has no pain in the left leg, no back pain, and the strength of the muscles in his left leg is much improved. The test for a pinched nerve is now negative.
Careful management in the future is vital to ensure that he doesn't just have a relapse in a couple months, and end up under the knife anyway.
- COMPLICATIONS OF SURGERY
- LOWER BACK SURGERY; when to consult a specialist.
Chiropractic help for sciatic pain
Patients with sciatica is a daily occurrence in every chiropractic clinic. Even medical research now grudgingly admits that manipulation is the treatment of choice for lumbago with leg pain.
Once it goes down your leg you do have to take it seriously, follow your chiropractor's instructions faithfully and do basic exercises daily, preferably for the rest of your life. Just like you brush your teeth.
Exercises
The sacroiliac joint is frequently involved in lower back conditions. In chronic cases, it is inclined to subluxate repeatedly. A simple set of exercises for SIJ pain, as well as lumbago with radiation into the leg is essential.

It's encouraging to find a general medical textbook, widely used in Australia, that is pro-chiropractic. There is now strong medical research confirming that manipulation is the treatment of choice for acute and chronic lower back and leg pain.
- MURTAGH'S GENERAL PRACTICE ...
LUMBAR FACET ARTHROPATHY causes low back pain with extension of the spine.
Spinal stenosis explanation may shed further light on your problem should you have unremitting lumbago with leg pain.
When browsing these links use right click and "Open Link in New Tab", or you may get a bad gateway signal.
- Home
- SLIPPED DISC
- Lumbago with leg pain
Did you find this page useful? Then perhaps forward it to a suffering friend. Better still, Tweet or Face Book it.
